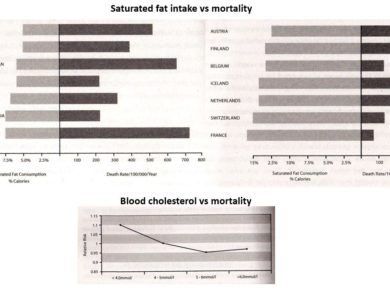
There is no direct evidence that chemotherapy prolongs survival in patients with advanced carcinoma.
Dr. Abel says:
“there is no scientific evidence for its ability to extend in any appreciable way the lives of patients suffering from the most common organic cancer. Chemotherapy for malignancies too advanced for surgery, which accounts for 80% of all cancers, is a scientific wasteland.”
“Chemotherapy of advanced epithelial cancer–a critical review.”
https://www.ncbi.nlm.nih.gov/pubmed/1339108
You can also read his book:
“cytostatic chemotherapy of advanced epithelial tumors: a critical inventory” published in 1995.
Another paper confirms this:
The contribution of cytotoxic chemotherapy to 5-year survival in adult malignancies.
https://www.ncbi.nlm.nih.gov/pubmed/15630849
The authors state:
“the overall contribution of curative and adjuvant cytotoxic chemotherapy to 5-year survival in adults was estimated to be 2.3% in Australia and 2.1% in the USA.”
Chemotherapy is clearly ineffective and actually dangerous.
But some people would say that the new targeted therapies are better and more effective.
But several papers show that is not the case
Assessment of Overall Survival, Quality of Life, and Safety Benefits Associated With New Cancer Medicines.
https://www.ncbi.nlm.nih.gov/pubmed/28033447
“They say:
Of the 62 new active cancer molecules approved by the FDA and EMA between 2003 and 2013, 53 were appraised by English, French, or Australian HTA agencies through May 2015. Of these 53 drugs, 23 (43%) increased OS by 3 months or longer, 6 (11%) by less than 3 months, and 8 (15%) by an unknown magnitude; there was no evidence to suggest that the remaining 16 (30%) increased OS over best alternative treatments. Where overall survival gains could be quantified, all new cancer drugs were associated with a mean (SE) total increase in OS of 3.43 (0.63) months over the treatments that were available in 2003. Drug-related improvements in OS were, however, widely distributed across therapeutic targets-ranging between 0 (thyroid, ascites) and 8.48 months (breast cancers)-and were sometimes based on modeled data, indirect or nonactive comparisons, or nonvalidated evidence. Although 22 (42%) of 53 new medicines were associated with an increase in QoL, 24 (45%) were also associated with reduced patient safety. Of the 53 new cancer drugs, 42 (79%) were associated with at least some improvement in OS, QoL, or safety.”
In other words, the authors have doubt about the effectiveness of those new cancer therapies.
Another paper is worth looking at:
“Availability of evidence of benefits on overall survival and quality of life of cancer drugs approved by European Medicines Agency: retrospective cohort study of drug approvals 2009-13.”
https://www.ncbi.nlm.nih.gov/pubmed/28978555
The authors conclude:
“This systematic evaluation of oncology approvals by the EMA in 2009-13 shows that most drugs entered the market without evidence of benefit on survival or quality of life. At a minimum of 3.3 years after market entry, there was still no conclusive evidence that these drugs either extended or improved life for most cancer indications. When there were survival gains over existing treatment options or placebo, they were often marginal.”
We can see that both old and new cancer therapies are completely useless in improving quality of life of patients and to extend their lives.
But what about breast cancer?
I hear all the time that if you have the BRCA mutations, you are at higher risk of having cancer. This is another myth that is not supported by scientific evidence.
Let’s look into this misconception.
Germline BRCA mutation and outcome in young-onset breast cancer (POSH): a prospective cohort study
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5805863/
The authors state:
“We found no clear evidence that either BRCA1 or BRCA2 germline mutations significantly affect overall survival with breast cancer after adjusting for known prognostic factors.”
“The POSH prospective cohort study showed no significant difference in overall survival or distant disease-free survival between patients carrying a BRCA1 or BRCA2 mutation and patients without these mutations after a diagnosis of breast cancer.”
Here’s another paper to read:
Worse breast cancer prognosis of BRCA1/BRCA2 mutation carriers: what’s the evidence? A systematic review with meta-analysis.
https://www.ncbi.nlm.nih.gov/pubmed/25816289
They researchers conclude:
“In contrast to currently held beliefs of some oncologists, current evidence does not support worse breast cancer survival of BRCA1/2 mutation carriers in the adjuvant setting; differences if any are likely to be small.”
This paper is very interesting because they demonstrate that some variations of these gene may be in fact protective.
“The case against BRCA 1 and 2 testing.”
https://www.ncbi.nlm.nih.gov/pubmed/21621683
The author state:
“a variation in K1183R is related inversely to cancer risk. It seems that some polymorphisms may actually have a protective effect.”
Then, the next question is: should women be screened for breast cancer?
The answer is: there is no evidence that it improves survival rates or quality of life.
Likelihood That a Woman With Screen-Detected Breast Cancer Has Had Her “Life Saved” by That Screening
https://jamanetwork.com/journals/jamainternalmedicine/article-abstract/1106067
The conclusion:
“Most women with screen-detected breast cancer have not had their life saved by screening. They are instead either diagnosed early (with no effect on their mortality) or overdiagnosed.”
Quantifying the benefits and harms of screening mammography.
https://www.ncbi.nlm.nih.gov/pubmed/24380095
This is what the researchers have to say:
“Among 1000 US women aged 50 years who are screened annually for a decade, 0.3 to 3.2 will avoid a breast cancer death, 490 to 670 will have at least 1 false alarm, and 3 to 14 will be overdiagnosed and treated needlessly.”
Effect of Three Decades of Screening Mammography on Breast-Cancer Incidence
https://www.nejm.org/doi/full/10.1056/NEJMoa1206809
Conclusion:
“Despite substantial increases in the number of cases of early-stage breast cancer detected, screening mammography has only marginally reduced the rate at which women present with advanced cancer. Although it is not certain which women have been affected, the imbalance suggests that there is substantial overdiagnosis, accounting for nearly a third of all newly diagnosed breast cancers, and that screening is having, at best, only a small effect on the rate of death from breast cancer.”
Effect of screening on ovarian cancer mortality: the Prostate, Lung, Colorectal and Ovarian (PLCO) Cancer Screening Randomized Controlled Trial.
https://www.ncbi.nlm.nih.gov/pubmed/21642681
Conclusion:
“Among women in the general US population, simultaneous screening with CA-125 and transvaginal ultrasound compared with usual care did not reduce ovarian cancer mortality. Diagnostic evaluation following a false-positive screening test result was associated with complications.”
CA-125 is a marker of ovarian cancer.
Prostate cancer diagnosis and treatment after the introduction of prostate-specific antigen screening: 1986-2005.
https://www.ncbi.nlm.nih.gov/pubmed/19720969
“The introduction of PSA screening has resulted in more than 1 million additional men being diagnosed and treated for prostate cancer in the United States. The growth is particularly dramatic for younger men. Given the considerable time that has passed since PSA screening began, most of this excess incidence must represent overdiagnosis.”
The Natural History of Invasive Breast Cancers Detected by Screening Mammography
https://jamanetwork.com/journals/jamainternalmedicine/fullarticle/773446
The authors conclude:
“Because the cumulative incidence among controls never reached that of the screened group, it appears that some breast cancers detected by repeated mammographic screening would not persist to be detectable by a single mammogram at the end of 6 years. This raises the possibility that the natural course of some screen-detected invasive breast cancers is to spontaneously regress.”
In other words, cancer found by screening exam can and do go away on their own.
We should not be afraid of cancer, because we can prevent it! Yes, a good diet, supplements, appropriate lifestyle changes are the key to cancer prevention.
2 Corinthians 4:16-19
“Therefore we do not lose heart. Though outwardly we are wasting away, yet inwardly we are being renewed day by day. For our light and momentary troubles are achieving for us an eternal glory that far outweighs them all. So we fix our eyes not on what is seen, but on what is unseen, since what is seen is temporary, but what is unseen is eternal.”
God bless y’all 😊
Dr. Serge